Why Estradiol Levels Matter
Estradiol levels are one of the central data points in evaluating menopause, perimenopause, fertility, and hormone therapy. Estradiol is the most potent of the three estrogens the body produces and the one that drops dramatically in midlife. Knowing where your level sits — and how it relates to your symptoms — helps determine whether hormone therapy is appropriate and at what dose.
Important caveat: a single estradiol blood result is rarely the full picture. The same level can be normal in one woman and symptomatic in another, depending on the rate of decline, individual receptor sensitivity, and the time of day, cycle, or recent HRT dose at which the sample was drawn. Lab values inform, but symptoms guide treatment.
Normal Estradiol Levels by Age and Phase (Chart)
Reference ranges vary slightly between labs and assay methods (liquid chromatography–mass spectrometry vs. immunoassay). The values below reflect the most commonly cited US laboratory ranges for serum estradiol.
| Stage / phase | Estradiol (pg/mL) | Notes |
|---|---|---|
| Prepubertal girls | < 15 | Below adult ranges before puberty begins |
| Early follicular phase (days 1–5) | 30–60 | Lowest point in the cycle outside the luteal nadir |
| Mid-follicular (days 6–10) | 50–150 | Rising estradiol prepares the endometrium |
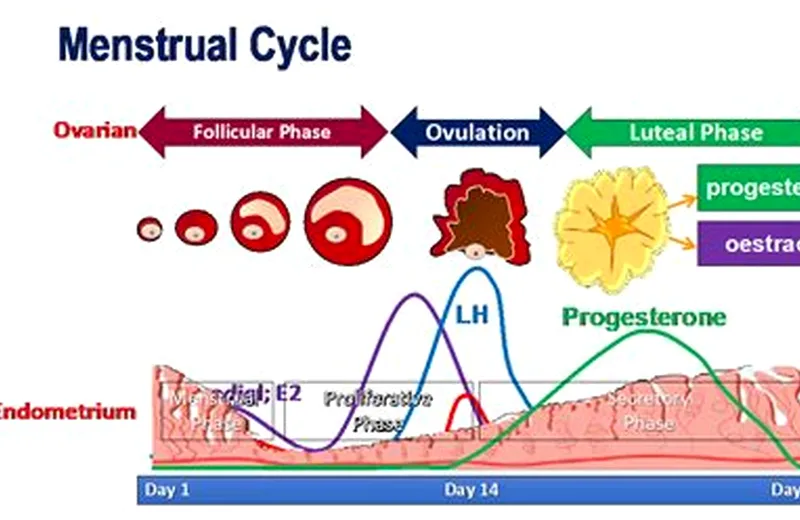
| Late follicular / ovulation peak | 150–400 | Pre-ovulatory surge, triggers LH |
| Luteal phase (days 15–28) | 70–250 | Secondary peak supports possible implantation |
| Perimenopause | Highly variable | Can range from < 10 to > 300 within months |
| Postmenopausal (no HRT) | < 30 (often < 10) | Ovarian production has essentially ceased |
| On transdermal estradiol HRT (typical target) | 40–100 | Adjusted to symptom relief, not a fixed target |
| Pregnancy (first trimester) | 200–4,000 | Continuously rising |
| Pregnancy (third trimester) | 5,000–20,000+ | Placental production |
Values shown are typical reference ranges and should not be used to self-diagnose. Your individual lab report will include its own reference intervals — those are the ones to compare against.
Estradiol Levels in Perimenopause
Perimenopause is the 4–10 years before menopause when ovarian function becomes erratic. Cycles shorten, lengthen, and skip; estradiol surges and crashes unpredictably. A blood test on the wrong day can read like a 25-year-old's; the next week's draw can look postmenopausal.
This volatility — not low levels themselves — is the engine behind many perimenopausal symptoms: hot flashes, sleep disruption, anxiety, mood swings, and heavy or irregular periods. The estradiol level on any given day is less important than the pattern of swings and the symptom burden.
Clinicians evaluating perimenopause usually combine:
- A detailed symptom history
- Cycle pattern over the last 12 months
- FSH and estradiol — sometimes on multiple days
- TSH, prolactin, and other hormones to rule out other causes
- Anti-Müllerian hormone (AMH) for ovarian reserve, if relevant
Estradiol Levels in Menopause
Menopause is defined as 12 consecutive months without a menstrual period. By that point, ovarian estradiol production has essentially ceased; most circulating estrogen is now estrone, made by fat tissue from adrenal precursors.
Typical postmenopausal estradiol values are under 30 pg/mL, often under 10 pg/mL. This is the deficiency state that hormone therapy aims to address. On estradiol replacement therapy, many clinicians target levels in the 40–80 pg/mL range — high enough to relieve symptoms and protect bone, low enough to stay within the physiologic envelope of premenopausal early follicular phase.
Some women feel best at higher levels (80–150 pg/mL). Some are symptom-free at lower levels. There is no single "right" estradiol level on HRT. The clinician adjusts dose against symptoms, side effects, and risk.
How Estradiol Is Tested
Estradiol can be measured by:
- Serum blood draw — standard, lab-grade, most common. Best for most clinical decisions.
- Finger-prick capillary blood — used in at-home test kits; accurate when collected correctly.
- Saliva — measures free (unbound) hormone. Useful for some research but generally less standardized for clinical use.
- Dried urine (DUTCH testing) — captures hormone metabolites over 24 hours; useful for evaluating estrogen metabolism patterns, not for tracking everyday HRT dose response.
For HRT dose adjustment, serum or capillary blood drawn at a consistent time relative to the dose is most useful. For a patch, sample any time during the wearing window. For oral estradiol, sample at the same time of day each visit (often 4–6 hours after the dose).
What Affects Your Estradiol Level
- Age and menopause status — by far the largest driver
- Day of menstrual cycle — premenopausal women
- HRT regimen and timing of last dose
- Body fat — fat tissue makes estrone, mildly raising total estrogen
- Liver function — affects clearance
- Thyroid status — alters SHBG and bound vs. free fractions
- Alcohol use — heavy alcohol raises levels modestly
- Certain medications — including some birth-control pills and aromatase inhibitors
Get a real reading of your hormone levels.
Skip the doctor-office runaround. A free assessment plus an at-home hormone kit can clarify whether your symptoms match your levels — and what to do about it.
Take Free Hormone AssessmentFree · No credit card required · Takes 3–5 minutes
How HRT Brings Estradiol Levels Back
Hormone replacement therapy is, mechanically, simple: you add back the estradiol your ovaries are no longer making. The route matters because each form produces a different blood-level pattern.
| Form | Typical level achieved | Pattern |
|---|---|---|
| 0.05 mg/day patch | 40–60 pg/mL | Steady, flat |
| 0.1 mg/day patch | 80–120 pg/mL | Steady, flat |
| 1 mg oral estradiol | 30–80 pg/mL peak, falling through the day | Peak and trough |
| 2 mg oral estradiol | 60–150 pg/mL peak | Peak and trough |
| Vaginal cream (low dose) | Minimal systemic rise | Mostly local |
These are population averages. Individual absorption varies — some women on the same patch produce double or half the typical blood level. That is why post-dose testing is useful when symptoms are not responding as expected.
What It Costs
Transparent flat-rate care. No insurance billing, no surprise charges.
First month
$29 /mo
Then
$99/mo
- Unlimited video and message visits with hormone-trained clinicians
- At-home hormone testing kit included
- Personalized bioidentical estradiol regimen (patch, cream, or oral)
- Free discreet shipping every month
- Cancel any time — no contracts, no fees
Free, no-obligation assessment first. Treatment plan offered only if clinically appropriate.
