What Is Estradiol?
Estradiol is the primary form of estrogen in women of reproductive age and the most potent of the three estrogens the body produces. It is a steroid hormone made mainly by the ovaries from cholesterol, with smaller amounts produced in fat tissue and the adrenal glands. Estradiol is also written as 17β-estradiol or simply E2.
Estradiol drives the development of female secondary sex characteristics at puberty, regulates the menstrual cycle, and keeps tissues across the body running on their default settings. It binds to estrogen receptors (ERα and ERβ) in the brain, bone, cardiovascular system, skin, urogenital tract, breast, joints, liver, and adipose tissue. When estradiol falls during perimenopause and menopause, the systems it was quietly supporting begin to compensate — and many of those compensations show up as menopausal symptoms.
In modern medicine, "estradiol" most often refers to the bioidentical hormone used in hormone replacement therapy (HRT). It comes in patches, gels, creams, tablets, injections, and vaginal rings or tablets. All FDA-approved estradiol products contain the same active molecule — what changes is how it gets into the body.
Estradiol vs. Estrogen — What's the Difference?
This is the most common point of confusion. "Estrogen" is the family name for a group of related hormones, and "estradiol" is one specific member of that family. Saying you are taking estrogen is like saying you are eating fruit; saying you are taking estradiol is like saying you are eating an apple.
The three principal estrogens in women:
- Estradiol (E2) — most potent. Dominant from puberty through perimenopause. The standard form used in modern HRT.
- Estrone (E1) — less potent. Becomes the predominant estrogen after menopause, produced mainly by fat tissue from adrenal precursors.
- Estriol (E3) — weakest. Produced mainly by the placenta during pregnancy and is largely irrelevant outside of pregnancy.
Other "estrogens" you may have heard of are not human estrogens at all: conjugated equine estrogens (CEE), like Premarin, are a mixture of estrogens extracted from pregnant mare urine. Ethinyl estradiol, used in most birth control pills, is a synthetic modification of estradiol designed to survive first-pass liver metabolism. Both behave differently from bioidentical estradiol and have different risk profiles.
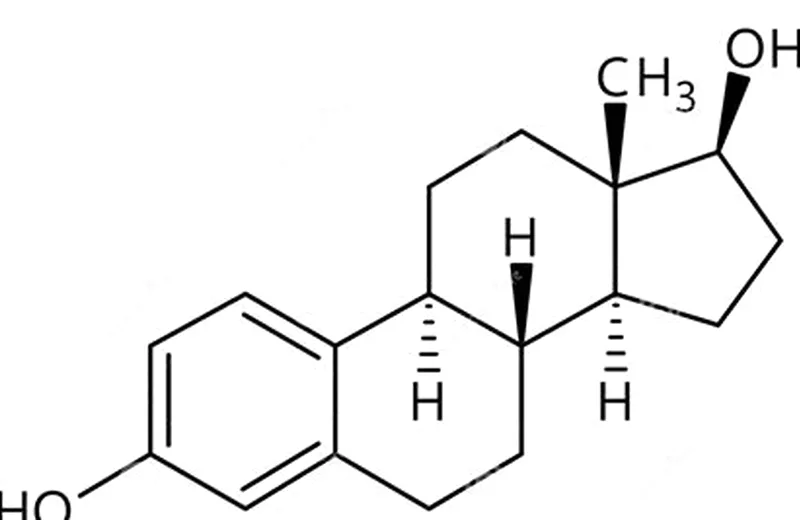
Estriol vs. Estradiol
Two estrogens, different roles. Estradiol is roughly 80 times more potent than estriol at the estrogen receptor. Estradiol dominates a woman's reproductive years; estriol surges only during pregnancy.
In clinical use:
- Estradiol — the standard systemic HRT hormone. Patches, gels, pills, creams, rings. Treats hot flashes, sleep, mood, bone density.
- Estriol — appears mainly in compounded vaginal estrogen preparations and some European HRT products. Used for vaginal symptoms when minimal systemic absorption is desired. Not FDA-approved as a stand-alone systemic HRT in the US.
Some compounded "Biest" formulas combine the two (typically 80% estriol, 20% estradiol). They are popular in certain wellness clinics but are not standardized and are not FDA-approved. Most evidence-based menopause care defaults to FDA-approved estradiol.
What Does Estradiol Do?
Estradiol's reach is extraordinarily broad. A non-exhaustive map of what it does in the female body:
Reproductive System
Drives the menstrual cycle. Stimulates growth of the uterine lining each cycle. Maintains vaginal epithelium thickness, lubrication, and elasticity. Supports breast tissue development and cyclical changes.
Brain and Cognition
Modulates serotonin, dopamine, and acetylcholine signalling. Influences mood, sleep, memory, focus, and verbal fluency. Plays a role in temperature regulation in the hypothalamus (which is why dropping estradiol causes hot flashes). Estrogen receptors are densely distributed in the hippocampus, prefrontal cortex, and thermoregulatory centers.
Bone
Inhibits osteoclast activity, slowing bone resorption. When estradiol drops at menopause, bone turnover accelerates and women can lose 2–5% of bone density per year for the first few years. This is the central mechanism behind menopausal osteoporosis.
Cardiovascular System
Improves HDL cholesterol, lowers LDL, helps blood vessels dilate, and supports endothelial function. The protective effect is part of why premenopausal women have lower cardiovascular disease rates than men of the same age — and why cardiovascular risk rises after menopause.
Skin and Hair
Maintains collagen production, skin thickness, hydration, and elasticity. Slows hair thinning. Many of the visible changes of menopause — drier skin, thinner hair, slower wound healing — track estradiol decline.
Urinary Tract
Keeps the urethra and bladder lining healthy. Estradiol deficiency causes urinary urgency, frequency, recurrent UTIs, and the rest of genitourinary syndrome of menopause.
Metabolism and Fat Distribution
Influences insulin sensitivity and where the body stores fat. Premenopausal women carry fat preferentially on the hips and thighs; postmenopausal women shift toward abdominal storage. Restoring estradiol modestly reverses this pattern.
Wondering if low estradiol is behind your symptoms?
A free 3-minute hormone assessment with a licensed clinician can answer that. They look at your symptoms, history, and (if needed) lab work to decide whether estradiol therapy makes sense for you.
Take Free Hormone AssessmentFree · No credit card required · Takes 3–5 minutes
What Is Estradiol Used For?
FDA-approved uses for estradiol include:
- Vasomotor symptoms of menopause — hot flashes and night sweats.
- Vulvovaginal atrophy / genitourinary syndrome of menopause — dryness, painful intercourse, recurrent UTIs.
- Prevention of postmenopausal osteoporosis — when other therapies are not appropriate.
- Female hypoestrogenism — after oophorectomy, premature ovarian insufficiency, or as primary care for women in surgical menopause.
- Gender-affirming care — feminizing hormone therapy.
Common off-label uses include support during fertility treatment cycles and certain aspects of brain and cardiovascular health protection in early postmenopausal women.
How Estradiol Works as a Medication
Modern estradiol therapy gives your body the same molecule it stopped producing. Several routes exist because each one delivers the hormone differently:
- Transdermal patch — steady delivery through skin, bypasses liver.
- Vaginal cream — mostly local, minimal systemic absorption.
- Oral tablet — convenient; passes through liver first, slightly higher clot risk.
- Topical gel or spray — transdermal alternative to patches.
- Vaginal ring — three months of low-dose delivery.
- Injection — less common, longer interval, higher peaks.
Once estradiol enters circulation it binds to estrogen receptors throughout the body and restores the signalling that was missing. Symptoms relief follows a predictable timeline — hot flashes within 2–4 weeks, sleep within 2–3 weeks, mood and cognition within 4–12 weeks, vaginal symptoms within 8–12 weeks of local or systemic therapy.
Estradiol Levels and the Menstrual Cycle
Estradiol is the architect of the menstrual cycle. In the early follicular phase (days 1–5) it sits low. As a dominant follicle develops, estradiol rises sharply, triggering the LH surge that causes ovulation. In the luteal phase, the corpus luteum produces a secondary estradiol peak alongside progesterone. If pregnancy does not occur, both hormones fall and menstruation begins.
Normal cycling estradiol ranges from roughly 30 pg/mL in early follicular phase to 200–400 pg/mL at the mid-cycle peak. Detailed reference values are on the estradiol levels chart page.
Estradiol After Menopause
After menopause, ovarian estradiol production essentially ceases. Circulating estrogen drops by roughly 90% and shifts toward the weaker estrone, made by fat tissue. The decline is not subtle — many women's serum estradiol falls from a cycling 100–200 pg/mL to under 10 pg/mL within a year of their final menstrual period. That deficiency is what HRT with estradiol is designed to address.
What It Costs
Transparent flat-rate care. No insurance billing, no surprise charges.
First month
$29 /mo
Then
$99/mo
- Unlimited video and message visits with hormone-trained clinicians
- At-home hormone testing kit included
- Personalized bioidentical estradiol regimen (patch, cream, or oral)
- Free discreet shipping every month
- Cancel any time — no contracts, no fees
Free, no-obligation assessment first. Treatment plan offered only if clinically appropriate.
